By Jeffrey McNerney
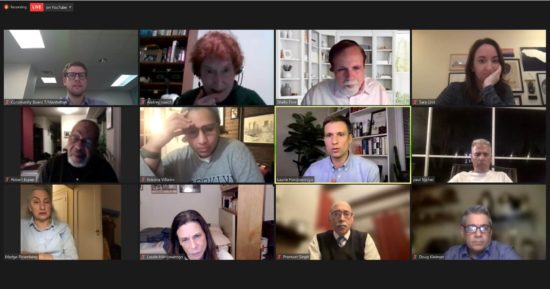
With recent high-profile tragedies drawing headlines and attention, the issue of mental health, particularly among the unhoused, has been a major consideration for UWS residents and elected officials. Members of both groups came together to focus on the problem at Tuesday’s meeting of Community Board 7’s Health & Human Services Committee.
The virtual meeting chaired by Shelly Fine began with a discussion led by newly elected Council Member Erik Bottcher from Manhattan’s District 3. CM Bottcher, who made mental health issues the centerpiece of his campaign, said, “You don’t need to walk far down the streets of New York City to see people suffering from untreated mental illness….” Making it clear that the issue is a personal one for him, Bottcher shared his experience of being involuntarily committed after suicide attempts as a closeted teen and credited the intervention with saving his life.
Bottcher’s comments centered on the proposals he laid out in a recent editorial for the New York Daily News. These included reversing the closure of inpatient psychiatric beds and the creation of more medical-respite beds for those healthy enough to leave the hospital but requiring further treatment before returning to shelters or the street. He also emphasized the need for organizations like Fountain House in Hell’s Kitchen, which follow a “clubhouse model” of providing community for those with serious mental illness. “At a basic level,” said the Councilmember, “people need things to do all day.” Finally, he called for a revamp of discharge planning for the incarcerated. He called the current process “a joke” and told stories of former inmates he spoke with who hadn’t even been assigned a social worker.
Committee members were supportive of Bottcher’s proposals in the discussion that followed, and Chair Fine suggested drafting a resolution in support of Bottcher’s proposals, which was passed unanimously at the end of the meeting. Fine then introduced Dr. Prameet Singh, Associate Professor of Psychiatry and Chair of the Department at Mount Sinai Morningside and West Hospitals, who contributed a perspective from the medical community. He noted that while he hasn’t seen a shortage of inpatient beds in the city specifically, he agreed the key is what happens after patients receive treatment and how to avoid a revolving door of admission and release.
Describing changes he’s seen in the last couple of years due to COVID, Dr. Singh said there have been both setbacks and opportunities. Many patients undergoing treatment became disconnected during the pandemic, and he’s also seen an increase in psychiatric emergency room visits for children and teens whose struggles may have gone unnoticed during the last two years. Bright spots include the relaxation of in-person requirements for social services and treatment, which, he said, led to an increase in patients with addictions and children being able to keep appointments.
After Dr. Singh’s discussion, the virtual floor opened to community members. Several Upper Westsiders spoke favorably of their experiences with the system when it worked, but said that strict requirements, lack of funding, and uncertainty led to a lack of confidence.
One resident asked what ordinary community members could do to help, which led Chair Fine to introduce Pastor James Payne who credited a national training program, called “Mental Health First Aid,” with helping people learn to observe changes in those they’re close to, offer a non-judgmental ear, and provide early intervention if necessary. He announced a partnership with the organization CASES which will be offering the training for free.
For further details, the full meeting is available here.








Useless.
You’re not allowed to say that anymore.
Just as political correctness now requires us to shun the description “homeless” in favor of “unhoused” (as in the above article), we should now avoid all of the negative connotations attached to “useless” and instead use the more neutral, less charged “unused”.
Better get with it!
You got me good there Cato.
They’re on right track but need to go further.
A significant number of persons with serious & persistent mental illness &/ substance abuse disorders resist engagement in treatment. In such instances it will be necessary to invoke Kendra’s Law (outpatient involuntary commitment) which requires adherence to a treatment plan & provides expedited access to services. Also, more drug courts should be created & utilized – those involved with drug court programs avoid incarceration as long as they adhere to agreed upon care plans.
An approach which combines compassion while firmly requiring adherence to treatment is our best bet for addressing the behavioral deviance which has become widely endemic our communities.
This past week, walking north from 96th to 100th Street on Broadway, I encountered no less than 7 panhandlers. In some cases there were 2 on a block. It seems much more prevalent than below 96th Street. I don’t know if these people are mentally ill or not, homeless or not, etc. Some were standing, others sitting on the street with some possessions.
I suspect what they all had in common is that they were poor.
Every Saturday morning, when I pass the church on the SE corner of 93rd St. & B’way, I see people lined up to get free food. None of them are panhandling, & none appear to be either mentally ill or homeless.